Journal Description
Diabetology
Diabetology
is an international, peer-reviewed, open access journal on diabetes research published quarterly online by MDPI.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within ESCI (Web of Science), Scopus, EBSCO, and other databases.
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 18 days after submission; acceptance to publication is undertaken in 6.8 days (median values for papers published in this journal in the second half of 2023).
- Journal Rank: CiteScore - Q2 (Medicine (miscellaneous))
- Recognition of Reviewers: APC discount vouchers, optional signed peer review, and reviewer names published annually in the journal.
Impact Factor:
2.4 (2023);
5-Year Impact Factor:
2.4 (2023)
Latest Articles
Overweight and Obesity in Adults with Type 1 Diabetes: A Growing Challenge
Diabetology 2024, 5(3), 234-245; https://doi.org/10.3390/diabetology5030018 - 24 Jun 2024
Abstract
The prevalence of obesity in adults with type 1 diabetes is increasing and reflects the rates of the general adult population. The coexistence of overweight or obesity and type 1 diabetes poses a major challenge to effective glycemic and weight management. In addition,
[...] Read more.
The prevalence of obesity in adults with type 1 diabetes is increasing and reflects the rates of the general adult population. The coexistence of overweight or obesity and type 1 diabetes poses a major challenge to effective glycemic and weight management. In addition, individuals living with T1D and overweight or obesity are at greater cardiometabolic risk and are more prone to develop chronic complications in comparison to normal weight individuals with type 1 diabetes. Although obesity represents a growing challenge in the type 1 diabetes population, awareness of this issue is still low. This review provides a summary of current data on prevalence trends, causes, current strategies, and challenges in managing obesity in adults with type 1 diabetes.
Full article
Open AccessArticle
The Utility of Annual Reassessment of the International Working Group on the Diabetic Foot Diabetes-Related Foot Ulcer Risk Classification in the Primary Care Setting—A Cohort Study
by
Matilde Monteiro-Soares, José Dores, Cristina Alves-Palma, Susana Galrito and Daniela Ferreira-Santos
Diabetology 2024, 5(2), 223-233; https://doi.org/10.3390/diabetology5020017 - 4 Jun 2024
Abstract
Background: We assessed the pertinence of updating the International Working Group on the Diabetic Foot (IWGDF) risk classification yearly in people with diabetes by quantifying the changes in the risk group and its accuracy in identifying those developing an ulcer (DFU) in a
[...] Read more.
Background: We assessed the pertinence of updating the International Working Group on the Diabetic Foot (IWGDF) risk classification yearly in people with diabetes by quantifying the changes in the risk group and its accuracy in identifying those developing an ulcer (DFU) in a primary care setting. Methods: In our retrospective cohort study, we included all people with diabetes with a foot assessment registry between January 2016 and December 2018 in the Baixo Alentejo Local Health Unit. Foot-related data were collected at baseline after one and two years. DFU and/or death until December 2019 were registered. The proportion of people changing their risk status each year was calculated. Accuracy measures of the IWGDF classification to predict DFU occurrence at one, two, and three years were calculated. Results: A total of 2097 people were followed for three years, during which 0.1% died and 12.4% developed a DFU. After two years, 3.6% of the participants had progressed to a higher-risk group. The IWGDF classification presented specificity values superior to 90% and negative predictive values superior to 99%. Conclusion: Foot risk status can be safely updated every two years instead of yearly, mainly for those at very low risk. The IWGDF classification can accurately identify those not at risk of DFU.
Full article
(This article belongs to the Special Issue Exclusive Papers Collection of Editorial Board Members in Diabetology)
►▼
Show Figures

Figure 1
Open AccessArticle
A Resource-Efficient Plantar Pressure Evaluation System for Diabetic Foot Risk Assessment
by
Madison Reddie and Daniel Frey
Diabetology 2024, 5(2), 206-222; https://doi.org/10.3390/diabetology5020016 - 22 May 2024
Abstract
►▼
Show Figures
Diabetic foot complications constitute a large and rapidly growing global health problem, causing one million lower-extremity amputations annually. These amputations are typically preceded by preventable diabetic foot ulcers (DFUs). However, 80% of the world’s diabetics now reside in low- and middle-income countries, where
[...] Read more.
Diabetic foot complications constitute a large and rapidly growing global health problem, causing one million lower-extremity amputations annually. These amputations are typically preceded by preventable diabetic foot ulcers (DFUs). However, 80% of the world’s diabetics now reside in low- and middle-income countries, where many healthcare settings lack the resources required to implement recommended DFU risk assessment and prevention strategies. There is an unmet need for a more resource-efficient DFU risk assessment method. In this study, a low-cost, purely mechanical plantar pressure evaluation device was designed toward this end. The device consists of a grid of plastic bistable compliant mechanisms, which present a visual series of binary outputs in response to applied pressure. By having diabetic patients step on the device, non-specialist healthcare providers can easily assess patients’ plantar pressures, which are predictive of future DFUs. A prototype was fabricated and pilot-tested with 41 healthy subjects. It demonstrated a sensitivity of 25.6%, although sensitivity reached 60% for heavier subjects. Sensitivity could likely be significantly improved by lowering the device’s profile and increasing the sensing area. Strained health systems may then be able to use this device to allocate scarce healthcare resources more efficiently to prevent costly DFUs and amputations.
Full article

Figure 1

Figure 3

Figure 4

Figure 5

Figure 6

Figure 7

Figure 8

Figure 9

Figure 10
Open AccessArticle
Prevalence of Peripheral Arterial Disease and Principal Associated Risk Factors in Patients with Type 2 Diabetes Mellitus: The IDON-Peripheral Arterial Disease Study
by
Aliyanet Isamara Porcayo Ascencio, Evangelina Morales Carmona, Jesús Morán Farías, Dulce Stephanie Guzmán Medina, Rebeca Galindo Salas and Leobardo Sauque Reyna
Diabetology 2024, 5(2), 190-205; https://doi.org/10.3390/diabetology5020015 - 14 May 2024
Abstract
The principal purpose of this study is to determine the prevalence of peripheral arterial disease (PAD), as well as the principal associated risk factors, in patients registered in the IDON-PAD database. PAD is a condition characterized by the narrowing or blockage of arteries
[...] Read more.
The principal purpose of this study is to determine the prevalence of peripheral arterial disease (PAD), as well as the principal associated risk factors, in patients registered in the IDON-PAD database. PAD is a condition characterized by the narrowing or blockage of arteries in the body’s extremities due to plaque buildup, leading to reduced blood flow and tissue ischemia. While PAD primarily affects the lower extremities, it can lead to symptoms such as intermittent claudication and, in severe cases, ulcers and amputations. Risk factors for PAD are numerous and cumulative, including smoking, age over 50, type 2 diabetes mellitus, and hypertension. The prevalence of PAD increases with age, with rates ranging from 2.5% in those over 50 to 60% in those over 85, varying by ethnicity and study population. Diabetic patients face a higher risk of PAD-related complications and have lower success rates with revascularization procedures. The diagnosis of PAD traditionally relied on physical examination and symptoms, but the Ankle–Brachial Index is now a standard diagnostic tool due to its non-invasive nature and reliability. In Mexico, the prevalence of PAD is estimated at 10%, with significant risk factors being the duration of diabetes, hypertension, hypertriglyceridemia, and smoking. Notably, 70% of PAD cases are asymptomatic, emphasizing the importance of proactive screening. This study aimed to determine the prevalence of PAD and associated risk factors in diabetic patients aged 40 and above. The prevalence was found to be 11.2%, with high-risk waist circumference, elevated triglycerides, positive Edinburgh questionnaire, and weak pulses as significant predictors. The detection and management of PAD in diabetic patients require a comprehensive approach, including lifestyle modifications and regular screenings. Prevention strategies should focus on controlling risk factors, including obesity, hypertension, and dyslipidemia. In conclusion, PAD is a prevalent yet underdiagnosed condition in diabetic patients, necessitating proactive screening and comprehensive management to mitigate associated risks and improve patient outcomes. The principal limitation of this study is that, as it uses a cross-sectional methodology and is not an experimental study, although we can establish the prevalence of PAD as well as the associated risk factors, we cannot define causality or determine the hazard ratio for each of these factors. Special thanks to Dr. Leobardo Sauque Reyna and all participants for their contribution to this research.
Full article
(This article belongs to the Special Issue Feature Papers in Diabetology 2023)
►▼
Show Figures

Figure 1
Open AccessArticle
Defining the miRnome of Saphenous Vein Smooth Muscle Cells from Patients with Type 2 Diabetes Mellitus
by
Alisah Hussain, Yaw Asare-Amankwah, Shehryar Qureshi, M. Julie Thornton, Timothy M. Palmer, Israel O. Bolanle, Ian C. Wood, Neil A. Turner, Karen E. Porter, Andrew Tedder and Kirsten Riches-Suman
Diabetology 2024, 5(2), 178-189; https://doi.org/10.3390/diabetology5020014 - 11 May 2024
Abstract
Type 2 diabetes mellitus (T2DM) patients suffer premature development of cardiovascular disease and commonly require cardiac revascularization using the autologous saphenous vein (SV). Smooth muscle cells (SMCs) are the principal cell type within the vascular wall and are dysfunctional in T2DM SV-SMCs, yet
[...] Read more.
Type 2 diabetes mellitus (T2DM) patients suffer premature development of cardiovascular disease and commonly require cardiac revascularization using the autologous saphenous vein (SV). Smooth muscle cells (SMCs) are the principal cell type within the vascular wall and are dysfunctional in T2DM SV-SMCs, yet the mechanisms underpinning this are incompletely understood. The purpose of this study was to interrogate differential microRNA (miRNA) expression in SV-SMCs to enhance our understanding of T2DM SV-SMC phenotypic change. miRNA expression in primary human SV-SMCs from T2DM and non-diabetic (ND) donors was determined using an array (n = 6 each of ND and T2DM SV-SMCs). Differentially expressed miRNAs were ranked, and functional annotation of the 30 most differentially expressed miRNAs using DAVID and KEGG analysis revealed pathways related to SMC phenotype, including proliferation, migration, cytokine production and cell signaling. After selecting miRNAs known to be involved in SMC phenotypic regulation, miR-17, miR-29b-2, miR-31, miR-130b and miR-491 were further validated using qRT-PCR (n = 5 each of ND and T2DM SV-SMC), with miR-29b-2 subsequently being removed from further investigation. Potential mRNA targets were identified using mirDIP. Predicted target analysis highlighted likely dysregulation in transcription, epigenetic regulation, cell survival, intracellular signaling and cytoskeletal regulation, all of which are known to be dysfunctional in T2DM SV-SMCs. In conclusion, this paper identified four miRNAs that are dysregulated in T2DM SV-SMCs and are implicated in functional changes in the behavior of these cells. This provides a step forward in our understanding of the molecular and epigenetic regulation of vascular dysfunction in T2DM.
Full article
(This article belongs to the Special Issue Exclusive Papers Collection of Editorial Board Members in Diabetology)
►▼
Show Figures

Figure 1

Figure 3

Figure 4
Open AccessArticle
Do T2DM and Hyperglycaemia Affect the Expression Levels of the Regulating Enzymes of Cellular O-GlcNAcylation in Human Saphenous Vein Smooth Muscle Cells?
by
Israel O. Bolanle, Gillian A. Durham, James P. Hobkirk, Mahmoud Loubani, Roger G. Sturmey and Timothy M. Palmer
Diabetology 2024, 5(2), 162-177; https://doi.org/10.3390/diabetology5020013 - 25 Apr 2024
Abstract
Protein O-GlcNAcylation, a dynamic and reversible glucose-dependent post-translational modification of serine and threonine residues on target proteins, has been proposed to promote vascular smooth muscle cell proliferation and migration events implicated in vein graft failure (VGF). Therefore, targeting the enzymes (glutamine fructose-6P
[...] Read more.
Protein O-GlcNAcylation, a dynamic and reversible glucose-dependent post-translational modification of serine and threonine residues on target proteins, has been proposed to promote vascular smooth muscle cell proliferation and migration events implicated in vein graft failure (VGF). Therefore, targeting the enzymes (glutamine fructose-6P amidotransferase (GFAT), O-GlcNAc transferase (OGT), and O-GlcNAcase (OGA)) that regulate cellular O-GlcNAcylation could offer therapeutic options to reduce neointimal hyperplasia and venous stenosis responsible for VGF. However, it is unclear how type 2 diabetes mellitus (T2DM) and hyperglycaemia affect the expression of these enzymes in human saphenous vein smooth muscle cells (HSVSMCs), a key cell type involved in the vascular dysfunction responsible for saphenous VGF. Therefore, our aim was to assess whether T2DM and hyperglycaemia affect GFAT, OGT, and OGA expression levels in HSVSMCs in vitro. Expression levels of GFAT, OGT, and OGA were determined in low-passage HSVSMCs from T2DM and non-T2DM patients, and in HSVSMCs treated for 48 h with hyperglycaemic (10 mM and 25 mM) glucose concentrations, by quantitative immunoblotting. Expression levels of OGT, OGA, and GFAT were not significantly different in HSVSMC lysates from T2DM patients versus non-T2DM controls. In addition, treatment with high glucose concentrations (10 mM and 25 mM) had no significant effect on the protein levels of these enzymes in HSVSMC lysates. From our findings, T2DM and hyperglycaemia do not significantly impact the expression levels of the O-GlcNAcylation-regulating enzymes OGT, OGA, and GFAT in HSVSMCs. This study provides a foundation for future studies to assess the role of O-GlcNAcylation on VGF in T2DM.
Full article
(This article belongs to the Special Issue Risk of Type 2 Diabetes Mellitus: Cardiorenometabolic Syndrome and Its Components)
►▼
Show Figures
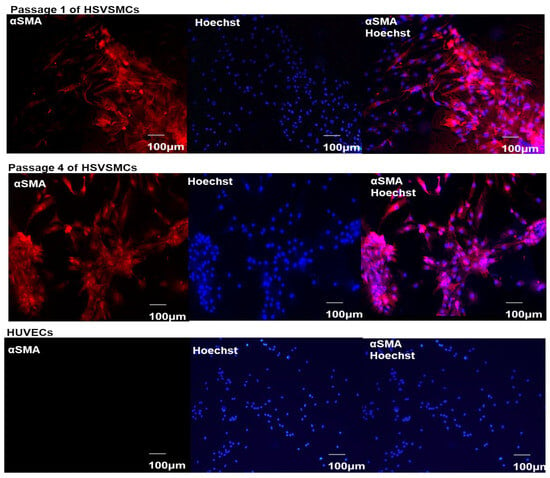
Figure 1
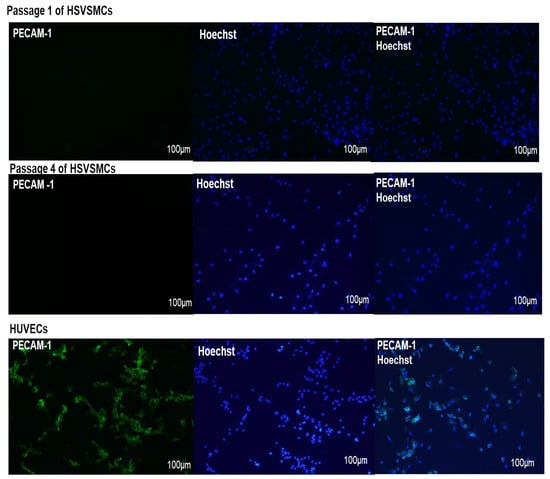
Figure 3
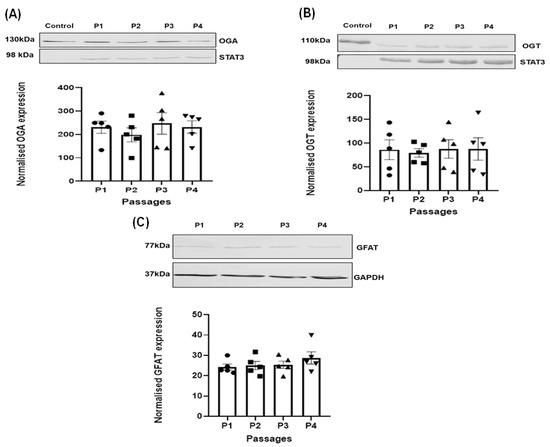
Figure 4
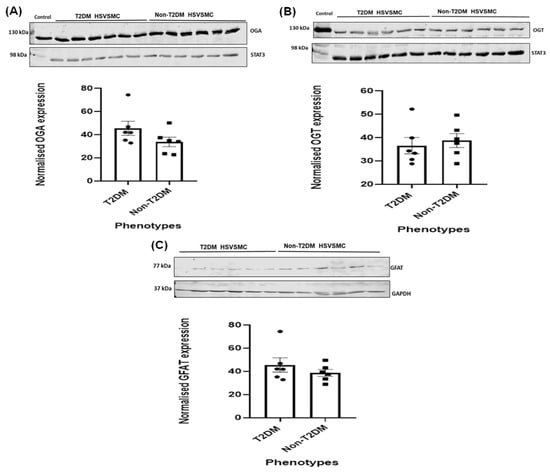
Figure 5
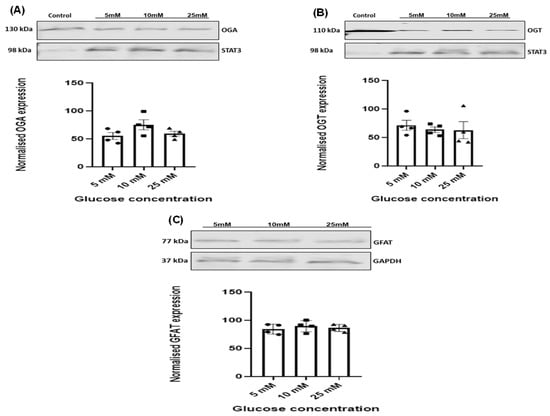
Figure 6
Open AccessArticle
Epidemiology of Diabetes Mellitus in Adults and Seniors in Rio Branco, Acre, Western Brazilian Amazon
by
Yara de Moura Magalhães Lima, Fernanda Andrade Martins and Alanderson Alves Ramalho
Diabetology 2024, 5(2), 151-161; https://doi.org/10.3390/diabetology5020012 - 10 Apr 2024
Abstract
►▼
Show Figures
(1) Background: To analyze the prevalence and factors associated with diabetes mellitus in adults and the elderly in Rio Branco, Acre, Western Brazilian Amazon. (2) Methods: The R software version 4.0.5 was used for estimating the prevalence of diabetes mellitus, odds ratios, and
[...] Read more.
(1) Background: To analyze the prevalence and factors associated with diabetes mellitus in adults and the elderly in Rio Branco, Acre, Western Brazilian Amazon. (2) Methods: The R software version 4.0.5 was used for estimating the prevalence of diabetes mellitus, odds ratios, and 95% confidence intervals. Multiple analysis was conducted through hierarchical variable selection. (3) Results: 1.095 individuals aged 18 years and older participated in this study, with 6.4% of the respondents showing prevalence of diabetes mellitus. The prevalence of diabetes mellitus was positively associated with a prior medical diagnosis of obesity (OR: 3.2; 95% CI: 1.67–6.12), dyslipidemia (OR: 4.17; 95% CI: 2.08–8.36), and increasing age (OR: 1.07; 95% CI: 1.05–1.09). Conversely, an inverse association was observed with higher education (12 or more years of study; OR: 0.20; 95% CI: 0.07–0.61). (4) Conclusions: The prevalence of diabetes mellitus in the municipality of Rio Branco, Acre, Brazil, has significantly increased with advancing age. Education, obesity, and dyslipidemia were also identified as factors associated with diabetes mellitus in this population. Awareness campaigns regarding dietary patterns and lifestyle choices may serve as preventive and control measures.
Full article
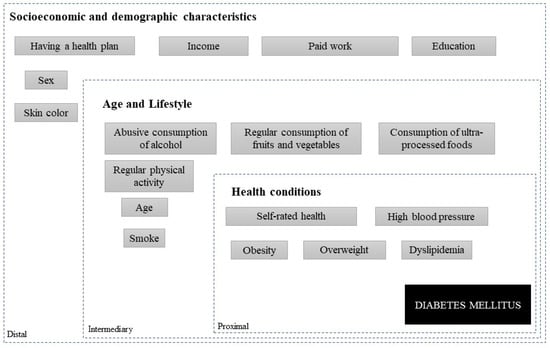
Figure 1
Open AccessArticle
Burden of Infected Diabetic Foot Ulcers on Hospital Admissions and Costs in a Third-Level Center
by
Roberto Da Ros, Roberta Assaloni, Andrea Michelli, Barbara Brunato, Enrica Barro, Marco Meloni and Cesare Miranda
Diabetology 2024, 5(2), 141-150; https://doi.org/10.3390/diabetology5020011 - 3 Apr 2024
Abstract
Diabetic foot is a common complication of diabetes that affects quality and prognosis of life for patients and often requires hospitalization. Infection, alone or in association with ischemia, is the main cause of hospital admission and impacts prognosis. The aim of this study
[...] Read more.
Diabetic foot is a common complication of diabetes that affects quality and prognosis of life for patients and often requires hospitalization. Infection, alone or in association with ischemia, is the main cause of hospital admission and impacts prognosis. The aim of this study is to analyze the costs of diabetic foot lesions and assess factors that influence the economic impact, focusing on infection. We included all people with diabetes with a first visit for diabetic foot during 2018 in our diabetic foot center. Database interrogation identified 422 patients. Diabetic foot treatment required hospitalization for 242 patients (58%), while 180 (42%) were treated in outpatient services. Healing time was different between the two groups: it was 136 ± 124 days (mean ± SD) for outpatients and 194 ± 190 days for patients that require hospitalization (p < 0.001). Costs: Treatment of 422 patients for diabetic foot globally costs 2063 million EUR and the mean cost for patients is 4888 EUR, with hospital stay having a high impact on this, accounting for 88% of the costs. Infection impacts hospitalization duration and ischemia impacts healing time. Ischemia and infection prolonged hospitalization duration and costs. Our work underlines that hospital treatment costs have a high impact on total costs.
Full article
(This article belongs to the Special Issue Feature Papers in Diabetology 2023)
Open AccessArticle
Utility of Flash Glucose Monitoring to Determine Glucose Variation Induced by Different Doughs in Persons with Type 2 Diabetes
by
Maria Antonietta Taras, Sara Cherchi, Ilaria Campesi, Valentina Margarita, Gavino Carboni, Paola Rappelli and Giancarlo Tonolo
Diabetology 2024, 5(1), 129-140; https://doi.org/10.3390/diabetology5010010 - 12 Mar 2024
Abstract
(1) Background: It has been previously shown that sourdough bread, compared to commercial yeast bread, elicits a lower postprandial glycemic and insulinemic response in patients with impaired glucose tolerance (IGT). Aims: Our aim was to evaluate the following aspects in persons with type
[...] Read more.
(1) Background: It has been previously shown that sourdough bread, compared to commercial yeast bread, elicits a lower postprandial glycemic and insulinemic response in patients with impaired glucose tolerance (IGT). Aims: Our aim was to evaluate the following aspects in persons with type 2 diabetes (T2DM): (1) glucose variations induced by three different doughs: X = bread prepared with functional alkaline biocrystal water, Y = sourdough-leavened bread, and W = bakery yeast bread; (2) the utility of flash glucose monitoring (FGM) to measure GL. (2) Methods: Twelve T2DM following diets (six males, diabetes duration 10.9 ± 1.3 years with no complications, Hba1c < 7.0%), after 12 h of fasting, consumed 180 g of the study breads leavened/matured for 48 (X), 8 (Y), and 4 h (W) at room temperature with 200 mL of water, in a random order, in single-blind conditions, on three different days. All patients had FGM running for the entire period of the experiments. Insulin was determined by capillary blood obtained for the basal and peak glucose concentrations. (3) Results: The peak glucose and peak insulin concentrations were significantly (p < 0.05) higher for W versus both X and Y, without significant differences between X and Y. The area under the curve of glucose variations for over 240 min was significantly higher in W than X (p < 0.01) and Y (p < 0.05), without significant differences between X and Y. (4) Conclusions: (1) Bread prepared with biocrystal water has the same lower GL of sourdough bread compared to bakery yeast bread, and it is easier to manage its leavening/maturation period; (2) FGM is a reliable method for determining rapid glucose changes in response to a carbohydrate meal in persons with type 2 diabetes.
Full article
(This article belongs to the Special Issue Feature Papers in Diabetology 2023)
►▼
Show Figures
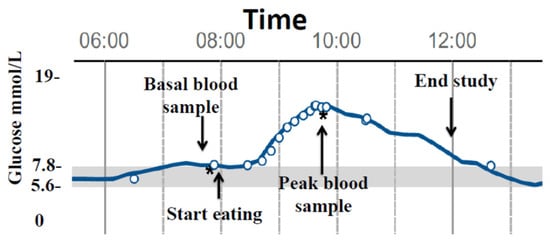
Figure 1
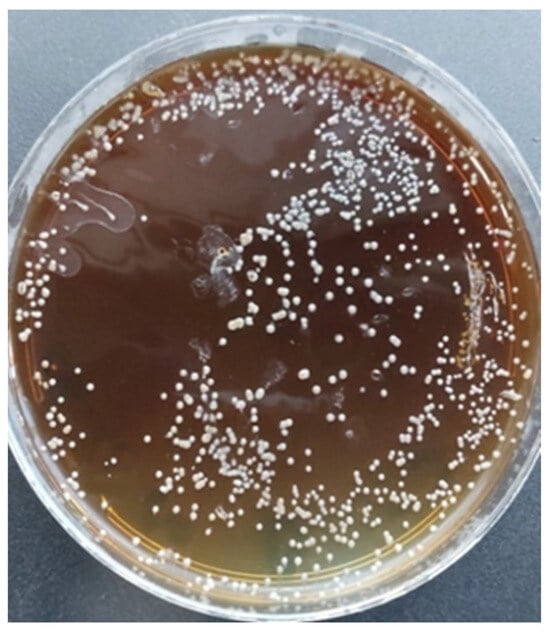
Figure A1

Figure A2
Open AccessArticle
Food as Medicine: FOODRx for Patients with Diabetes and Cardiovascular Disease in Central Minnesota—A PILOT STUDY
by
Mónica García-Pérez, Alexandra De Kesel Lofthus, David Tilstra, Kevin Switzer and Kristen Williamson
Diabetology 2024, 5(1), 110-128; https://doi.org/10.3390/diabetology5010009 - 8 Mar 2024
Abstract
►▼
Show Figures
The number of food-insecure individuals with diabetes is on the rise. FOODRx is a supplemental healthy food intervention program that gave disease-appropriate food boxes to food-insecure patients with diabetes at their care clinic and included nutrition and recipe materials in the patient’s preferred
[...] Read more.
The number of food-insecure individuals with diabetes is on the rise. FOODRx is a supplemental healthy food intervention program that gave disease-appropriate food boxes to food-insecure patients with diabetes at their care clinic and included nutrition and recipe materials in the patient’s preferred language (English, Spanish, or Somali). Implemented over a twelve-month period, we analyze FOODRx participants’ pre and post clinical measures, health care usage, and program/clinic satisfaction, and found that participation was linked to post improvements in fasting glucose and HgbA1c levels, reductions in ER visits and healthcare costs, and a decline in patients choosing between medication and food. Glucose levels decreased from 214 to 187 mg/dL and HgbA1c levels decreased from 9.6% to 9.1%. Average ER visits dropped from 1.21 to 1 visit and the reductions in healthcare costs were reflected in a decrease of an average of USD 250,000 in insurance claims. Patients were less likely to experience food insecurity, as measured in number of meals skipped and levels of hunger. Finally, the program improved patient satisfaction with the cultural responsiveness of the information shared with them.
Full article
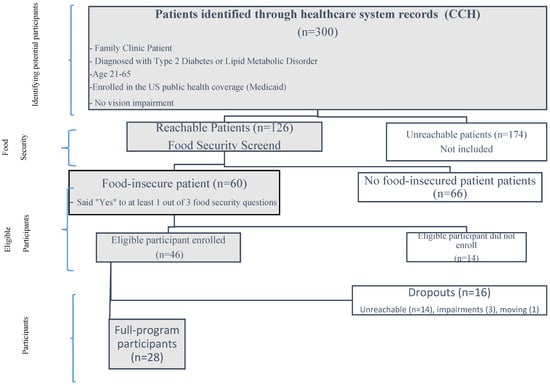
Figure 1
Open AccessArticle
Utilizing the Glucose and Insulin Response Shape of an Oral Glucose Tolerance Test to Predict Dysglycemia in Children with Overweight and Obesity, Ages 8–18 Years
by
Timothy J. Renier, Htun Ja Mai, Zheshi Zheng, Mary Ellen Vajravelu, Emily Hirschfeld, Diane Gilbert-Diamond, Joyce M. Lee and Jennifer L. Meijer
Diabetology 2024, 5(1), 96-109; https://doi.org/10.3390/diabetology5010008 - 1 Mar 2024
Abstract
Common dysglycemia measurements including fasting plasma glucose (FPG), oral glucose tolerance test (OGTT)-derived 2 h plasma glucose, and hemoglobin A1c (HbA1c) have limitations for children. Dynamic OGTT glucose and insulin responses may better reflect underlying physiology. This analysis assessed glucose and insulin curve
[...] Read more.
Common dysglycemia measurements including fasting plasma glucose (FPG), oral glucose tolerance test (OGTT)-derived 2 h plasma glucose, and hemoglobin A1c (HbA1c) have limitations for children. Dynamic OGTT glucose and insulin responses may better reflect underlying physiology. This analysis assessed glucose and insulin curve shapes utilizing classifications—biphasic, monophasic, or monotonically increasing—and functional principal components (FPCs) to predict future dysglycemia. The prospective cohort included 671 participants with no previous diabetes diagnosis (BMI percentile ≥ 85th, 8–18 years old); 193 returned for follow-up (median 14.5 months). Blood was collected every 30 min during the 2 h OGTT. Functional data analysis was performed on curves summarizing glucose and insulin responses. FPCs described variation in curve height (FPC1), time of peak (FPC2), and oscillation (FPC3). At baseline, both glucose and insulin FPC1 were significantly correlated with BMI percentile (Spearman correlation r = 0.22 and 0.48), triglycerides (r = 0.30 and 0.39), and HbA1c (r = 0.25 and 0.17). In longitudinal logistic regression analyses, glucose and insulin FPCs predicted future dysglycemia (AUC = 0.80) better than shape classifications (AUC = 0.69), HbA1c (AUC = 0.72), or FPG (AUC = 0.50). Further research should evaluate the utility of FPCs to predict metabolic diseases.
Full article
(This article belongs to the Special Issue Management of Type 2 Diabetes: Current Insights and Future Directions)
►▼
Show Figures
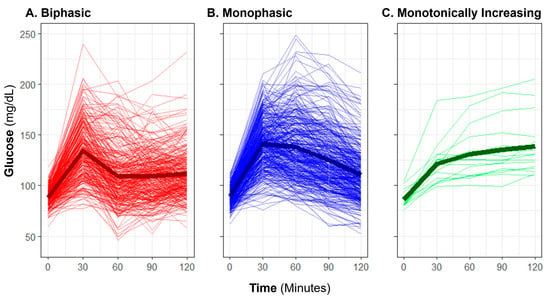
Figure 1
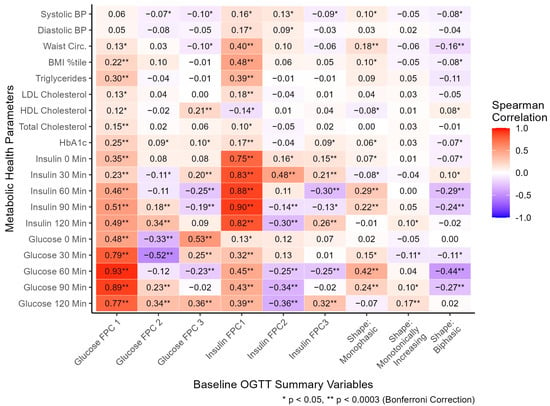
Figure 3
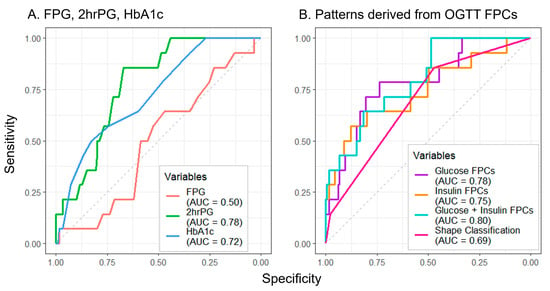
Figure 4