Journal Description
Transplantology
Transplantology
is an international, peer-reviewed, open access journal on all areas of experimental and clinical transplantation, published quarterly online by MDPI.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within Scopus, and other databases.
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 40.2 days after submission; acceptance to publication is undertaken in 5.7 days (median values for papers published in this journal in the second half of 2023).
- Recognition of Reviewers: APC discount vouchers, optional signed peer review, and reviewer names published annually in the journal.
- Transplantology is a companion journal of JCM.
Latest Articles
Bacterial Infections in End-Stage Liver Disease: Implications for Liver Transplantation
Transplantology 2024, 5(3), 129-139; https://doi.org/10.3390/transplantology5030013 - 28 Jun 2024
Abstract
Bacterial infections are a common complication in patients with decompensated liver cirrhosis. The complex landscape of cirrhosis, characterized by immune paralysis and an exhausted response to exogenous triggers, explains the higher prevalence of such infections, particularly in advanced disease stages. In clinical practice,
[...] Read more.
Bacterial infections are a common complication in patients with decompensated liver cirrhosis. The complex landscape of cirrhosis, characterized by immune paralysis and an exhausted response to exogenous triggers, explains the higher prevalence of such infections, particularly in advanced disease stages. In clinical practice, the onset of a bacterial infection can lead to further deterioration of hepatic and extra-hepatic function, potentially resulting in acute decompensation or acute-on-chronic liver failure. This has significant clinical implications, particularly for patients awaiting a transplant. In this review, we will discuss the latest evidence on the diagnosis and therapy of bacterial infections in patients with decompensated cirrhosis. Additionally, we will analyze the impact of bacterial infections in the context of liver transplantation, discussing debated topics such as the timing of transplantation in patients with infections, potential implications for prioritization, effects on post-operative recovery, grafts, and patient survival.
Full article
(This article belongs to the Section Perioperative Patient Management (i.e. Preabilitation, Intensive Care Management, Complications))
►
Show Figures
Open AccessReview
Evolving Biomarkers in Kidney Transplantation
by
Maurizio Salvadori, Alberto Rosati and Giuseppina Rosso
Transplantology 2024, 5(3), 116-128; https://doi.org/10.3390/transplantology5030012 - 21 Jun 2024
Abstract
Precision medicine is mainly based on reliable and noninvasive biomarkers. The aim of this review was to describe the newest biomarkers in the field of kidney transplantation and kidney rejection, one of the most common and severe complications. The standard tools used to
[...] Read more.
Precision medicine is mainly based on reliable and noninvasive biomarkers. The aim of this review was to describe the newest biomarkers in the field of kidney transplantation and kidney rejection, one of the most common and severe complications. The standard tools used to identify acute rejection largely result in errors and have many drawbacks. In recent years, new and reliable biomarkers have been identified. These methods avoid risks, are noninvasive, and are able to detect rejection even in cases in which acute rejection is clinically asymptomatic and not otherwise identifiable, which is a frequent occurrence. In recent years, several biomarkers have been identified. Very recently, new relevant biomarkers with high positive predictive value and low negative predictive value have been identified. These are the donor-derived cell-free DNA found in the recipient, the gene expression profile of the donor found in the recipient, and the urinary cytokines that are modified in the graft tissue. The aim of this study was to identify the most recent findings in the literature on this topic and to describe the utility and possible limitations of such new biomarkers for kidney rejection.
Full article
(This article belongs to the Collection Progress and Recent Advances in Solid Organ Transplantation)
►▼
Show Figures

Figure 1
Open AccessCase Report
Embolization of a Hepatic Arterio-Portal Venous Fistula to Treat Portal Hypertension in a Liver Transplant Recipient
by
Ji Ae Yoon, Cherng Chao and Zurabi Lominadze
Transplantology 2024, 5(2), 110-115; https://doi.org/10.3390/transplantology5020011 - 11 Jun 2024
Abstract
Hepatic arterio-portal venous fistula (HAPVF) is a rare, abnormal connection between the hepatic artery and portal vein. HAPVFs are usually caused by trauma or hepatobiliary instrumentation. Fistulas can expand and produce symptoms of severe portal hypertension. The decision to embolize should be based
[...] Read more.
Hepatic arterio-portal venous fistula (HAPVF) is a rare, abnormal connection between the hepatic artery and portal vein. HAPVFs are usually caused by trauma or hepatobiliary instrumentation. Fistulas can expand and produce symptoms of severe portal hypertension. The decision to embolize should be based on fistula location, size, and symptoms. We report a case of HAPVF in a liver transplant recipient presenting with worsening ascites and variceal hemorrhage after several prior liver biopsies. Given the extensive nature of the fistula and hepatic decompensation, the HAPVF was successfully embolized, resulting in clinical improvement and obviating the need for re-transplantation.
Full article
(This article belongs to the Section Solid Organ Transplantation)
►▼
Show Figures

Figure 1

Figure 3
Open AccessReview
Liver and Kidney Transplantation in Elderly Patients
by
John Guzzi, Eric Strand, Burhan Ozturk, Daniel Agarkov and Ranjit Deshpande
Transplantology 2024, 5(2), 98-109; https://doi.org/10.3390/transplantology5020010 - 31 May 2024
Abstract
►▼
Show Figures
Due to an aging population, advances in multiple medical fields, and shifts among indications for surgery, liver and kidney transplantation is increasingly pursued for elderly patients (aged 65 or greater). Elderly patients represent a uniquely vulnerable group, but overall, they appear to have
[...] Read more.
Due to an aging population, advances in multiple medical fields, and shifts among indications for surgery, liver and kidney transplantation is increasingly pursued for elderly patients (aged 65 or greater). Elderly patients represent a uniquely vulnerable group, but overall, they appear to have similar outcomes compared to younger patients. As demographics continue to trend to an older median age, physicians and health care systems must be prepared to take care of elderly transplant candidates.
Full article

Figure 1

Figure 3
Open AccessReview
Histocompatibility Testing: A Fundamental Aspect of Renal Transplant Workup
by
Vikash Chandra Mishra, Dinesh Chandra and Vimarsh Raina
Transplantology 2024, 5(2), 85-97; https://doi.org/10.3390/transplantology5020009 - 15 May 2024
Abstract
►▼
Show Figures
Histocompatibility testing is pivotal in any renal transplantation workup, aimed at enhancing prospective donor recipient compatibility and improving transplant outcomes. The evolution and advancement of histocompatibility testing, particularly HLA typing, have significantly improved its precision. This study outlines the historical progression from serologic
[...] Read more.
Histocompatibility testing is pivotal in any renal transplantation workup, aimed at enhancing prospective donor recipient compatibility and improving transplant outcomes. The evolution and advancement of histocompatibility testing, particularly HLA typing, have significantly improved its precision. This study outlines the historical progression from serologic to DNA-based HLA typing, emphasizing the role of HLA proteins in immune response. Anti-HLA antibodies, targeting HLA proteins, pose challenges in renal transplantation. Monitoring and managing these antibodies are critical for renal transplant success. Complement-dependent cytotoxicity crossmatch and flow cytometry crossmatch are essential techniques for assessing donor–recipient compatibility. Panel-reactive antibody assesses antibodies against a panel of donor antigens, often HLA. Higher PRA levels (percentage) complicate donor matching, requiring specialized protocols. Virtual crossmatch evaluates recipient anti-HLA antibodies against potential donors through synthetic beads. This approach predicts crossmatch outcomes by comparing antibody profiles, offering a valuable tool for the risk assessment of renal transplantation. Despite advancements, a comprehensive understanding of alloreactive immune responses requires a combination of assays, emphasizing the importance of a multifaceted approach in histocompatibility testing. This is an attempt to compile the relevant information, providing a basis for comparison in a clear and foundational format for histocompatibility testing laboratories.
Full article

Figure 1
Open AccessReview
Robotic Surgical Techniques in Transplantation: A Comprehensive Review
by
Marco Di Pangrazio, Federico Pinto, Alessandro Martinino, Francesco Toti, Gioia Pozza and Francesco Giovinazzo
Transplantology 2024, 5(2), 72-84; https://doi.org/10.3390/transplantology5020008 - 25 Apr 2024
Abstract
In the field of surgery, the idea of performing organ transplants in a minimally invasive fashion has always been a significant technical challenge. The advent of the robotic approach facilitated the overcoming of difficulties in highly complex surgical procedures that demand high technical
[...] Read more.
In the field of surgery, the idea of performing organ transplants in a minimally invasive fashion has always been a significant technical challenge. The advent of the robotic approach facilitated the overcoming of difficulties in highly complex surgical procedures that demand high technical skill. Furthermore, robotic transplants are showing significant benefits in patient outcomes, particularly in the obese population. The purpose of this review is to provide an overview of the current state of robotics applications for transplant surgery. Kidney transplants were the first to be performed using a fully robotic approach. Since then, robotic surgery has gradually been applied to other organ transplants, with very recent reports of fully robotic lung and liver transplants. Further experiences and studies will be needed to verify their effectiveness and to satisfy some concerns regarding the longer warm ischemia time related to the robotic approach in comparison with open surgery.
Full article
Open AccessCase Report
From Normal Renal Function to Renal Replacement Therapy after Liver Transplantation: A Case Report
by
Samuel Mangold, Gergely Albu, Julien Maillard, Florence Aldenkortt and Eduardo Schiffer
Transplantology 2024, 5(2), 65-71; https://doi.org/10.3390/transplantology5020007 - 11 Apr 2024
Abstract
Postoperative renal failure significantly impacts long-term renal function and the overall survival of patients receiving liver transplantation (LT), being a crucial factor in their morbidity and mortality. It is difficult to define whether the causes of renal failure are solely related to surgery
[...] Read more.
Postoperative renal failure significantly impacts long-term renal function and the overall survival of patients receiving liver transplantation (LT), being a crucial factor in their morbidity and mortality. It is difficult to define whether the causes of renal failure are solely related to surgery or anaesthesia during liver transplantation (LT). Indeed, liver disease requiring liver transplantation is often the cause of preoperative renal failure. We report a case of a 62-year-old patient undergoing LT for cholangiocarcinoma that led to acute kidney injury postoperatively while his preoperative renal function was normal. This report highlights the major influence that the surgical and anaesthetic procedure can have on renal function and identifies the factors that may have led to renal replacement therapy being required for this patient.
Full article
(This article belongs to the Collection Progress and Recent Advances in Solid Organ Transplantation)
Open AccessArticle
Wasted Potential: Decoding the Trifecta of Donor Kidney Shortage, Underutilization, and Rising Discard Rates
by
Ceilidh McKenney, Julia Torabi, Rachel Todd, M. Zeeshan Akhtar, Fasika M. Tedla, Ron Shapiro, Sander S. Florman, Matthew L. Holzner and L. Leonie van Leeuwen
Transplantology 2024, 5(2), 51-64; https://doi.org/10.3390/transplantology5020006 - 28 Mar 2024
Abstract
►▼
Show Figures
Kidney transplantation is a life-saving intervention for end-stage renal disease; yet, the persistent gap between organ demand and supply remains a significant challenge. This paper explores the escalating discard rates of deceased donor kidneys in the United States to assess trends, discard reasons,
[...] Read more.
Kidney transplantation is a life-saving intervention for end-stage renal disease; yet, the persistent gap between organ demand and supply remains a significant challenge. This paper explores the escalating discard rates of deceased donor kidneys in the United States to assess trends, discard reasons, demographical differences, and preservation techniques. Data from the Scientific Registry of Transplant Recipients from 2010 to 2021 was analyzed using chi-squared tests for trend significance and logistic regression to estimate odds ratios for kidney discard. Over the last decade, discard rates have risen to 25% in 2021. Most discarded kidneys came from extended criteria donor (ECD) donors and elevated kidney donor profile index (KDPI) scores. Kidney biopsy status was a significant factor and predictor of discard. Discard rates varied greatly between Organ Procurement and Transplantation Network regions. Of reasons for discard, “no recipient located” reached a high of 60%. Additionally, there has been a twofold increase in hypothermic machine perfusion (HMP) since 2010, with transportation difficulties being the main reason for the discard of perfused kidneys. Our findings suggest a need to recalibrate organ utilization strategies, optimize the use of lower-quality kidneys through advanced preservation methods, and address the evolving landscape of organ allocation policies to reduce kidney discard rates.
Full article
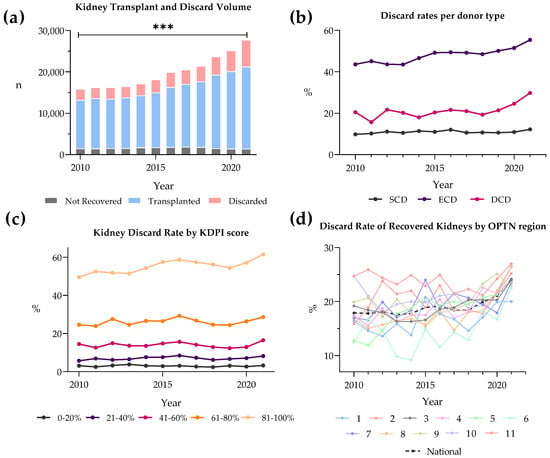
Figure 1
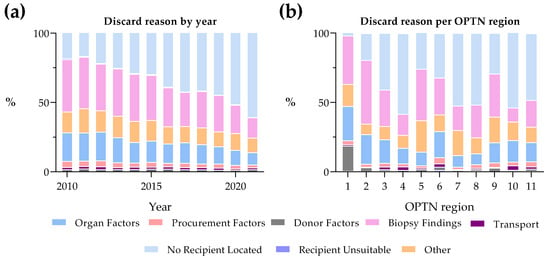
Figure 2
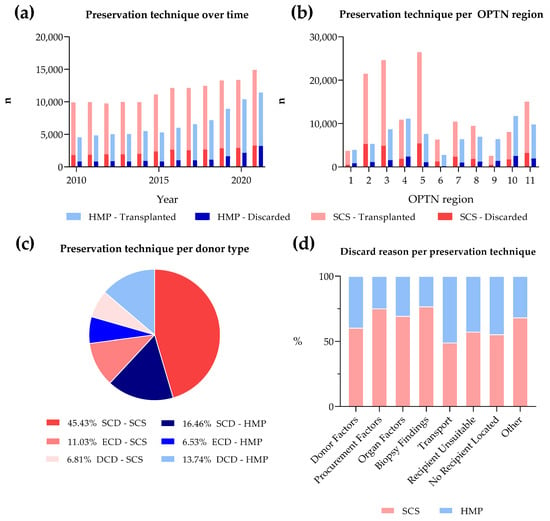
Figure 3
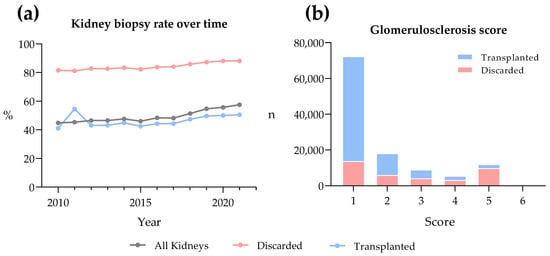
Figure 4
Open AccessBrief Report
Novel Study of SARS-CoV-2 RNA in Post-Reperfusion Liver Biopsies after Transplantation Using COVID-19-Positive Donor Allografts
by
Jenna N. Whitrock, Michela M. Carter, Adam D. Price, Aaron M. Delman, Catherine G. Pratt, Jiang Wang, Divya Sharma, Ralph C. Quillin III and Shimul A. Shah
Transplantology 2024, 5(1), 46-50; https://doi.org/10.3390/transplantology5010005 - 16 Mar 2024
Abstract
The utilization of COVID-19-positive donors has expanded the donor pool for transplantation since the initiation of COVID allograft utilization protocols. However, the biopsy-proven PCR transmission rate of COVID-19 from these allografts has not been well documented. In August 2021, an institutional COVID-19-positive allograft
[...] Read more.
The utilization of COVID-19-positive donors has expanded the donor pool for transplantation since the initiation of COVID allograft utilization protocols. However, the biopsy-proven PCR transmission rate of COVID-19 from these allografts has not been well documented. In August 2021, an institutional COVID-19-positive allograft protocol was implemented for liver and kidney transplants. Post-reperfusion liver biopsies were obtained intra-operatively to evaluate for COVID-19 RNA, and post-operative day 7 nasopharyngeal reverse transcriptase polymerase chain reaction (RT-PCR) swabs were collected. The primary endpoints evaluated included COVID-19 RNA on biopsy and COVID-19 detected via nasopharyngeal RT-PCR swab on post-operative day 7. A total of 20 vaccinated recipients underwent transplantation (17 liver only, 3 simultaneous liver and kidney) with whole liver allografts from 20 COVID-19-positive deceased donors between August 2021 and April 2022. 95% (19/20) of donors were asymptomatic at the time of donation. On post-reperfusion liver allograft biopsies, COVID-19 RNA was found in 10% (2/20) of the samples. All the recipients were COVID-19-negative on post-operative day 7 nasopharyngeal RT-PCR, showing a 0% transmission rate of COVID-19 from the positive allografts. The use of COVID-19 allografts appears to be a safe practice, with no PCR-detectable transmission of COVID-19 despite 10% of the liver allografts having COVID-19 RNA present on post-reperfusion biopsy.
Full article
Open AccessArticle
Pre-Emptive Kidney Retransplantation from Deceased Donors
by
Antonio Franco Esteve, Patricio Mas-Serrano, Fransico Manuel Marco, Eduardo Garin Cascales and Francisco Javier Perez Contreras
Transplantology 2024, 5(1), 37-45; https://doi.org/10.3390/transplantology5010004 - 28 Feb 2024
Abstract
There is uncertainty about the best approach to replacement treatment for kidney transplant recipients with chronic terminal graft dysfunction, since a retransplant could be performed before the resumption of dialysis, thus avoiding this treatment and the dilemma of whether or not to suspend
[...] Read more.
There is uncertainty about the best approach to replacement treatment for kidney transplant recipients with chronic terminal graft dysfunction, since a retransplant could be performed before the resumption of dialysis, thus avoiding this treatment and the dilemma of whether or not to suspend immunosuppressive therapy. However, there is limited experience in pre-emptive repeat transplantations, and none from deceased donors. This study aims to assess the results of a pre-emptive retransplantation program with brain-dead deceased donors. We designed a retrospective matched cohort study, including 36 recipients in the pre-dialysis group and 36 controls who were already on dialysis, matched for donor age and transplant date, which could not differ by more than 7 days between pairs. The variables used to standardize the cohorts were donor and recipient age and sex, blood group, duration of the first graft, time on the waitlist to receive the second graft, cold ischemia time, induction and maintenance of immunosuppression, and HLA antibodies (-) prior to retransplantation. The efficacy variables were early graft loss, acute rejection, delay in graft function, renal function at the end of follow-up, survival time, and recipient and graft survival at 24 and 48 months’ follow-up. The pre-dialysis group presented a significantly shorter waitlist time, lower immunization status, and a significantly longer duration of the first graft than the control group. The percentage of recipients who presented early graft loss, delayed renal function, or acute rejection was similar between groups. No significant differences were observed in kidney function or in the survival of the recipient or graft. Retransplantation yields good outcomes in patients with terminal chronic dysfunction, helping to avoid recurrence to dialysis, shortening the time spent on the waitlist, reducing the risk of producing antibodies, and resolving the dilemma of whether or not to stop immunosuppression.
Full article
(This article belongs to the Section Solid Organ Transplantation)
►▼
Show Figures
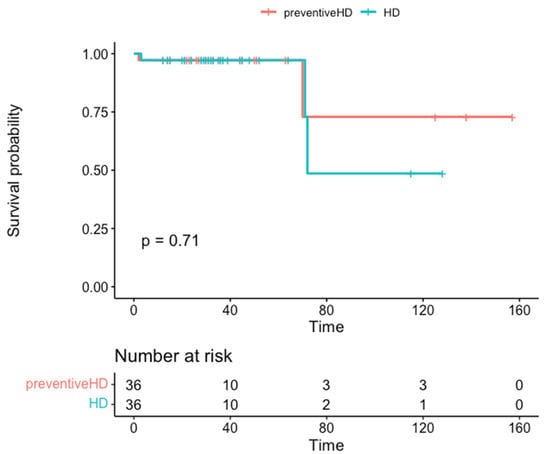
Figure 1
Open AccessArticle
Availability of Deceased Donors for Uterus Transplantation in the United States: Perception vs. Reality
by
Kathleen O’Neill, Elliott G. Richards, Jessica Walter, Sharon West, Richard Hasz, Giuliano Testa, Shreya Kalra, Tommaso Falcone, Rebecca Flyckt, Nawar Latif, Andreas Tzakis and Liza Johannesson
Transplantology 2024, 5(1), 27-36; https://doi.org/10.3390/transplantology5010003 - 4 Feb 2024
Abstract
►▼
Show Figures
Uterus transplantation (UTx) is a rapidly evolving treatment for uterine factor infertility. New centers offering this treatment must decide whether to utilize living donors, deceased donors, or both. Although limiting UTx to deceased donors eliminates the surgical risks for living donors, an adequate
[...] Read more.
Uterus transplantation (UTx) is a rapidly evolving treatment for uterine factor infertility. New centers offering this treatment must decide whether to utilize living donors, deceased donors, or both. Although limiting UTx to deceased donors eliminates the surgical risks for living donors, an adequate supply of suitable deceased uterus donors in the United States is an emerging concern. Previous studies describing the paucity of deceased uterus donors failed to consider key donor characteristics, potentially overestimating the available organ pool. To estimate the United States’ supply of deceased donor uteri; we extrapolated detailed clinical and demographic information from the regional donor datasets available from three organ procurement organizations to the national Organ Procurement and Transplantation Network donor pool. We estimate there are approximately 3700 possible and 400 optimal uterus donors annually in the United States. Given these projections and the number of women with uterine factor infertility in the U.S. who pursue parenthood through alternative strategies, we conclude that, as uterus transplant transitions from research to established clinical care, demand could quickly exceed the deceased donor supply. The liberalization of deceased donor selection criteria may be insufficient to address this imbalance; therefore, fulfilling the anticipated increased demand for uterus transplantation may require and justify greater use of living donors.
Full article
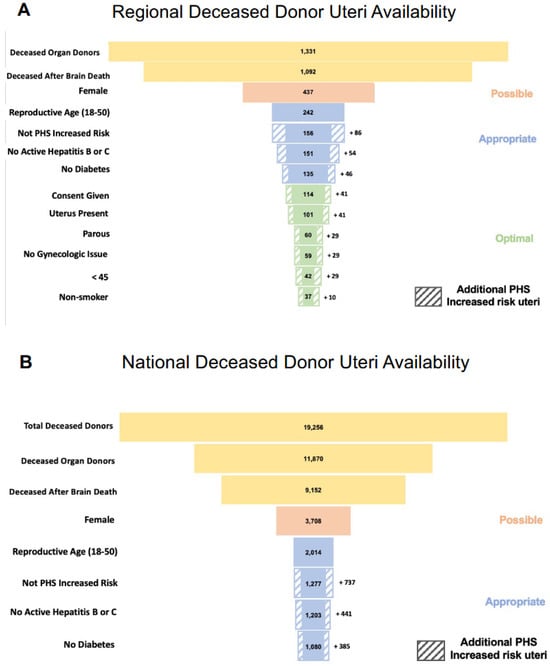
Figure 1
Open AccessArticle
Personality Changes Associated with Organ Transplants
by
Brian Carter, Laveen Khoshnaw, Megan Simmons, Lisa Hines, Brandon Wolfe and Mitchell Liester
Transplantology 2024, 5(1), 12-26; https://doi.org/10.3390/transplantology5010002 - 17 Jan 2024
Abstract
Personality changes have been reported following organ transplantation. Most commonly, such changes have been described among heart transplant recipients. We set out to examine whether personality changes occur following organ transplantation, and specifically, what types of changes occur among heart transplant recipients compared
[...] Read more.
Personality changes have been reported following organ transplantation. Most commonly, such changes have been described among heart transplant recipients. We set out to examine whether personality changes occur following organ transplantation, and specifically, what types of changes occur among heart transplant recipients compared to other organ recipients. A cross-sectional study was conducted in which 47 participants (23 heart recipients and 24 other organ recipients) completed an online survey. In this study, 89% of all transplant recipients reported personality changes after undergoing transplant surgery, which was similar for heart and other organ recipients. The only personality change that differed between heart and other organ recipients and that achieved statistical significance was a change in physical attributes. Differences in other types of personality changes were observed between these groups but the number of participants in each group was too small to achieve statistical significance. Overall, the similarities between the two groups suggest heart transplant recipients may not be unique in their experience of personality changes following transplantation, but instead such changes may occur following the transplantation of any organ. With the exception of physical attributes, the types of personality changes reported were similar between the two groups. These finding indicate that heart transplant recipients are not unique in their reported experience of personality changes following organ transplantation. Further studies are needed to deepen our understanding of what causes these personality changes.
Full article
(This article belongs to the Collection Progress and Recent Advances in Solid Organ Transplantation)
►▼
Show Figures
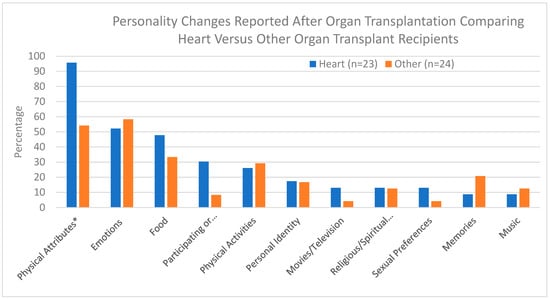
Figure 1